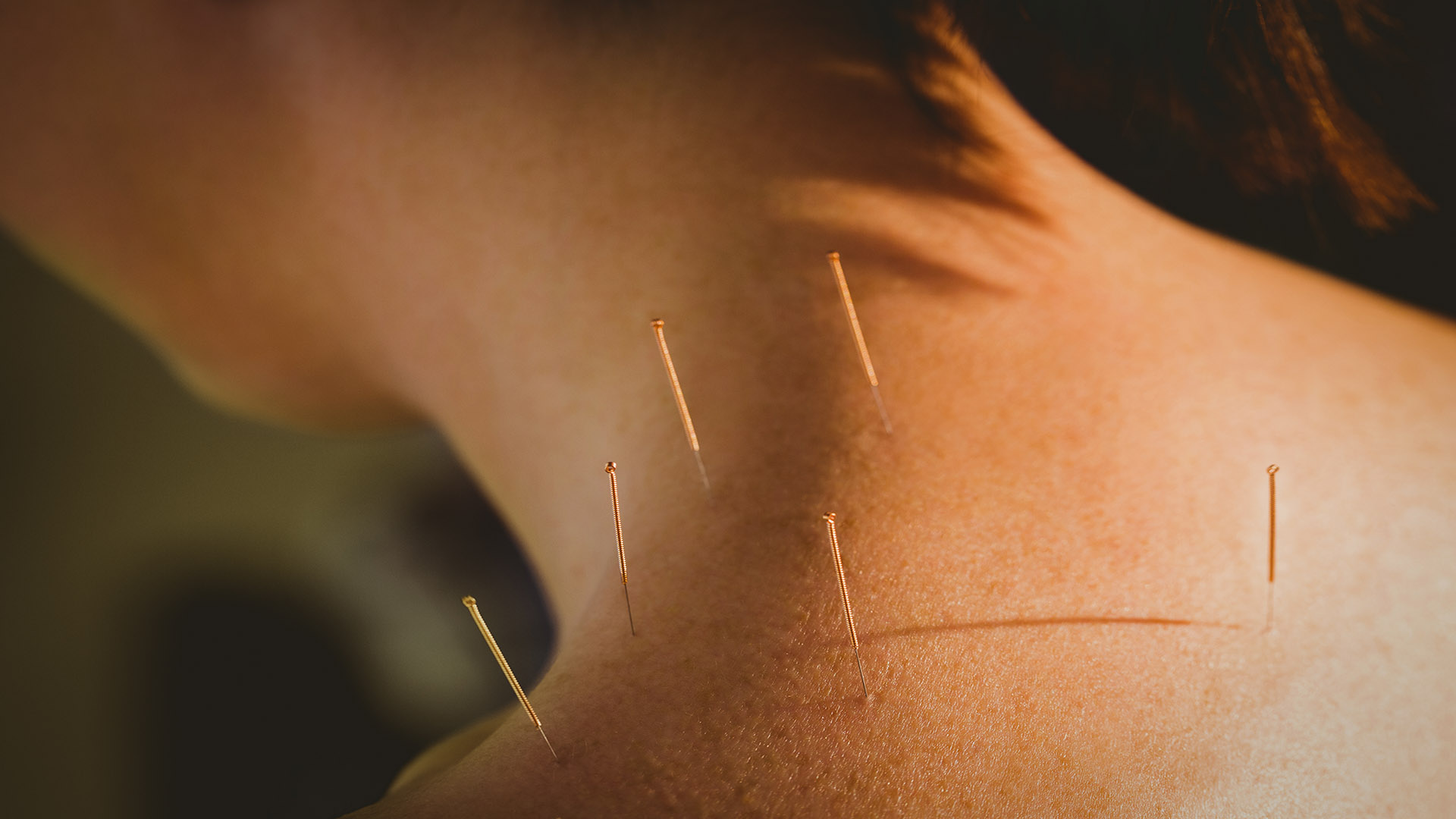
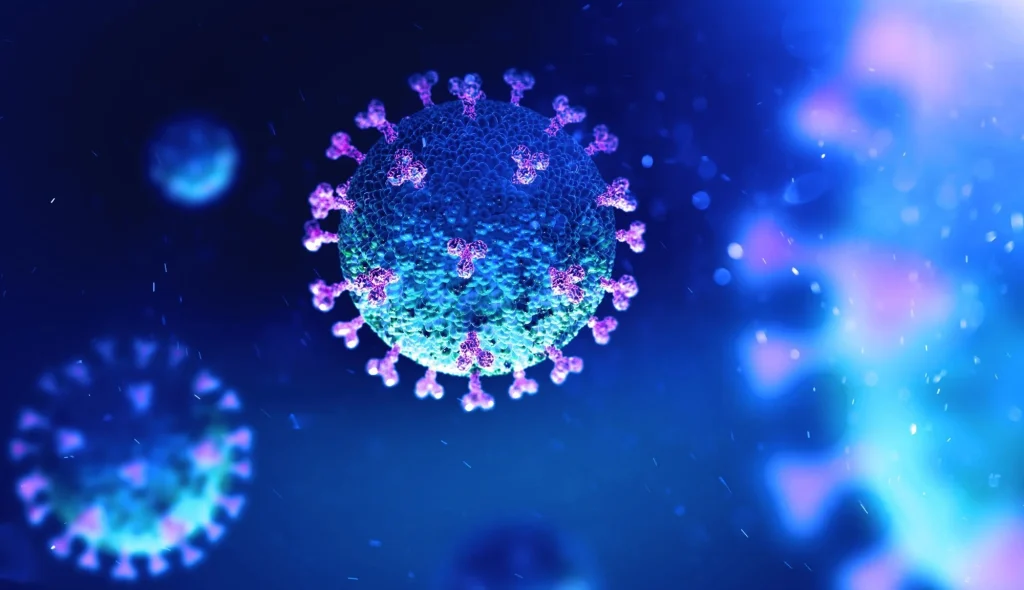
Navigating Long COVID Through a Functional Medicine Lens
As a Functional Medicine practitioner, I’ve seen rsthand how Long COVID—or Post-Acute Sequelae of SARS-CoV-2 (PASC)—can disrupt lives in profound and often unpredictable ways. This condition, characterized by a cluster of lingering symptoms long after the acute phase of COVID-19, has become a signicant focus of my practice.
Fatigue, brain fog, shortness of breath, joint pain, and mood disturbances are just a few of the challenges my patients face. Through a Functional Medicine lens, I’ve found that addressing the root causes of these symptoms can offer a personalized and effective path to recovery.

Understanding Long COVID
Long COVID isn’t a one-size-ts-all condition. In my practice, I’ve observed that symptoms can vary dramatically from person to person. Some patients struggle with persistent respiratory issues, while others battle debilitating fatigue or digestive problems. What ties these cases together is the underlying dysregulation—often involving chronic inammation, immune system confusion, and damage to various organ systems.
This variability is why a personalized approach is so critical. Functional Medicine allows us to dig deeper, uncovering the unique imbalances contributing to each patient’s symptoms.
The Functional Medicine Approach
In my work, I view Long COVID not as a single disease but as a manifestation of multiple physiological disruptions. My goal is always to identify and address these root causes, rather than simply managing symptoms. Here’s how I approach it:
1. Root Cause Exploration
I start by looking at the big picture. What’s happening in the gut? Are hormones out of balance? Are detoxication pathways functioning properly? Is the immune system struggling to reset? These are the kinds of questions I ask to uncover the deeper issues
at play.
2. Personalized Lab Testing
Comprehensive testing is a cornerstone of my practice. For Long COVID patients, I often recommend:
● Inammatory markers like CRP, IL-6, or brinogen to assess chronic
inammation.
● Immune proling to evaluate T-cell counts, immunoglobulins, and cytokine activity.
● Nutrient testing to identify deciencies in vitamins D, B12, iron, and other critical
micronutrients.
● Gut microbiome analysis to check for dysbiosis or pathogens that could be
contributing to systemic issues.
These tests provide a roadmap, guiding the development of a tailored treatment plan.
3. Key Strategies for Recovery
Based on the ndings, I work with my patients to implement targeted interventions.
Here are some of the strategies I often recommend:
● Reducing Inammation: Chronic inammation is a common thread in Long COVID. I often suggest an anti-inammatory diet rich in vegetables, fruits, lean proteins, and healthy fats. Supplements like omega-3 fatty acids and curcumin can also help calm inammatory pathways.
● Supporting Mitochondrial and Cellular Health: Many patients describe profound
fatigue and post-exertional malaise. To address this, I may recommend coenzyme Q10, NAD+ boosters, and antioxidants to support cellular energy production.
● Optimizing Gut Health: The gut is central to immune function, so I prioritize restoring gut health. Probiotics, prebiotics, and dietary changes can help rebalance the microbiome and strengthen the gut lining.
● Balancing Hormones: Stress-related hormones like cortisol often become dysregulated after severe illness. Adaptogenic herbs such as ashwagandha or rhodiola, combined with stress-management techniques, can help restore balance.
● Supporting Detoxication: For some patients, supporting liver and lymphatic function is key. Nutritional aids like milk thistle or glutathione precursors can enhance the body’s ability to clear toxins.
● Lifestyle Medicine: I always emphasize the importance of sleep, gentle exercise (like yoga or short walks), and stress reduction techniques such as mindfulness and breathwork. These foundational practices are essential for healing.
Collaborating with Patients
One of the most rewarding aspects of my work is the collaborative relationship I build with my patients. Together, we create a comprehensive plan that evolves as they progress. Regular check-ins and follow-up testing allow us to monitor improvements and make adjustments as needed.

Final Thoughts
Long COVID is undeniably complex, but it’s not insurmountable. Through Functional
Medicine, I’ve seen patients regain their energy, mental clarity, and overall wellness. By addressing the root causes and tailoring interventions to each individual, we can navigate this challenging condition with hope and condence.
If you’re struggling with Long COVID, know that you don’t have to face it alone. A
personalized, Functional Medicine approach can help you uncover the path to lasting recovery.